Can I Get Social Security Disability Benefits for Back Pain and Spine Immobility?
How Does the Social Security Administration Decide if I Qualify for Disability Benefits for Back Pain or Spine Impairments?
If you have a spine disorder that limits movement or causes chronic back pain, Social Security disability benefits may be available. To determine whether you are disabled by your back pain, or other spinal problems, the Social Security Administration first considers whether your back problems are severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process. See Winning Social Security Disability Benefits for Back Pain by Meeting a Listing. If you meet or equal a listing because of back pain or other spine disorders, you are considered disabled. If your back problems are not severe enough to equal or meet a listing, Social Security Administration must assess your residual functional capacity (RFC) (the work you can still do, despite your back), to determine whether you qualify for benefits at Step 4 and Step 5 of the Sequential Evaluation Process. See Residual Functional Capacity Assessment for Back Pain and Spine Impairments.
About Back Pain and Disability
Impairments Causing Back Pain and Spine Immobility
Allegations of disability based on “back pain” are extremely common. Back pain and movement problems may be caused by a number of disorders including:
- Osteoarthritis (OA)
- Degenerative disc disease (DDD)
- Herniated nucleus pulposus (HNP) or herniated disc
- Osteoporosis
- Trauma
- Tumor
- Arachnoiditis
- Lumbar strain
- Spondylolisthesis
- Spinal stenosis
- Scoliosis
- Kyphosis
- Osteomyelitis
Some people may have structural problems in the spine that limit function (i.e., walking, bending, stooping, etc.). But question of disability usually depends on how much your chronic pain interferes with your ability to function (i.e., walk, bend, stoop, twist, lift, etc.). The great majority of individuals—more than 80%—who have acute low back pain from a strain of the ligaments and other soft-tissue supportive structures of the spine will recover within several months, even if they receive no treatment. Other individuals have a more chronic problem.
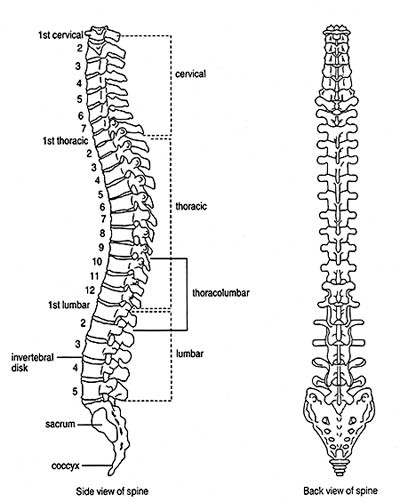
Spine Anatomy
The spine (vertebral column) has:
- 7 cervical (neck) vertebrae.
- 12 thoracic (chest, dorsal) vertebrae.
- 5 lumbar (lower back) vertebrae.
- 5 sacral vertebrae (fused triangular bone).
- 3 or 4 little vertebrae fused into a coccyx at the lower end of the spinal column.
The spine provides structural support for the body and protects the spinal cord. Thirty-one pairs of nerve roots exit the spinal cord to form the peripheral nerves to the rest of the body. The peripheral nerves are sensory (carrying sensation), and motor (causing muscle movement). Disease processes affecting the spine can damage peripheral nerves at or near their origin (nerve roots), as well as the spinal cord itself.
Assessing Back Pain
The severity of back pain cannot be deduced solely based on abnormalities that are seen on plain X-rays, computerized tomography (CT), or magnetic resonance imaging (MRI) of the spine. Many people with significant degenerative abnormalities on X-ray have minimal or no symptoms, while some people who allege incapacitating back pain have minimal objective abnormalities. Nevertheless, even taking individual differences into account, there is a general correlation between objective abnormalities and credible pain.
The Social Security Administration will weigh your objective abnormalities, your reported pain and other symptoms, and your credibility in determining the severity of your impairment. In addition to objective evidence, your credibility with the Social Security Administration is strongly influenced by your behavior in seeking relief of alleged symptoms, your activities that are limited by pain, the nature and frequency of your visits to a doctor for treatment, your response to treatment given, and comments about your credibility in the treating doctor’s records.
Psychological and Social Factors in Back Pain
Although psychosocial factors play a major role in the functional loss caused by low back pain, there is no good way for the Social Security Administration to evaluate these factors. Psychosocial factors strongly predict future disability and the use of health care services for low back pain. Chronic disabling low back pain develops more frequently in patients who, at the initial evaluation for low back pain, have:
- A high level of “fear avoidance” (an exaggerated fear of pain leading to avoidance of beneficial activities);
- Psychological distress;
- Disputed compensation claims;
- Involvement in a tort-compensation system; or
- Job dissatisfaction.
These psychosocial factors are particularly prevalent in persons with low back pain for whom imaging shows only degenerative changes; 70 to 80 percent of such patients demonstrate psychological distress on psychometric testing or have disputed compensation issues, compared with 20 to 30 percent of patients whose imaging studies reveal definite pathologic or destructive processes. These psychosocial factors should be routinely assessed in patients with low back pain and taken into account in decisions regarding treatment.
Osteoarthritis (OA)
Some degree of osteoarthritis of the spine is common in middle-aged people, even if they are not aware of it. OA of the spine can take several forms. In ankylosis, parts of the spine are abnormally fused together as a result of bony overgrowth. For example, bony spurs can fuse vertebral bodies together. The peripheral nerves formed from the spinal cord exit the bony spine through recesses in vertebrae called intervertebral foramina (see Figure 2 below). Some of these foramina can become encroached by osteoarthritis and require surgical decompression. Vertebrae have contact points with other vertebra called facet joints (see Figure 3 below).Arthritis affecting these facet joints can be painful and limit the motion of the spine. See also Can I Get Social Security Disability Benefits for Arthritis and Joint Damage?
Degenerative Disc Disease (DDD)
Degenerative disc disease refers to dehydration and shrinkage of the intervertebral discs that cushion the vertebral bodies of the spine. DDD is common and causes no symptoms in many older individuals. Everyone over about the age of 50 has some degree of DDD, which may or may not be symptomatic and functionally limiting. Osteoarthritis of the spine is frequently accompanied by DDD, while DDD without associated OA is also common. DDD can be seen on X-rays, MRI, and CT scans of the spine. It appears as narrowing of the space between vertebral bodies. Symptomatic DDD occurs between the 5th lumbar vertebra and the 1st sacral vertebra (L5-S1).
Sometimes a combination of OA and DDD produces enough symptoms that surgical fusion is performed in the lumbar spine (lumbar fusion) or cervical spine (neck). This procedure is done in an attempt to stabilize the spine and decrease pain. The surgery requires taking strips of bone from the posterior (back) upper part of the pelvic bone and laying them over the vertebral bodies that need to be stabilized (see Figure 4 below). Bone is living tissue and will incorporate the vertebral bodies into one solid mass. Sometimes, the bone strips do not incorporate well and the surgical fusion partially or wholly fails. Some fusions involve only two vertebrae, but multiple vertebrae may also be fused.
Herniated Nucleus Pulposus (HNP) or Herniated Disc
A herniated nucleus pulposus is the protrusion of the hard, cartilaginous center (nucleus) of an intervertebral disk through the outer fibrous tissue (annulus fibrosa) (see Figures 5 and 6 below). Many small HNPs will produce acute symptoms that improve with time. Injection of corticosteroid drugs in the area of the HNP can also help relieve inflammation and pain. Some claimants have a large HNP that presses on a spinal nerve root, and must have part of the HNP removed (discectomy, diskectomy).
Often, a part of a vertebral body, the lamina, is also removed for surgical access and this procedure is known as a laminectomy. The problem with surgery around spinal nerve roots is that manipulation of tissues often leads to scarring that then again pressures the nerve root. This is particularly likely when a person has had multiple back surgeries. Many claimants who complain of chronic back pain and have a history of back surgery near nerve roots have scarring that can be identified on CT or MRI scans. In the absence of trauma, most HNPs occur in the lumbar (lower) spine, especially at the level of L5-S1.
Osteoporosis
Osteoporosis is a metabolic disorder associated with decrease in the mass of bone. By far, most of the instances of osteoporosis seen by the Social Security Administration are in post-menopausal women. Osteoporosis may be confined to the spine, but other bones may be involved in those who have used corticosteroids. A collapse of vertebral bodies, especially in the upper back, is known as a compression fracture. Compression fractures are visible on plain X-ray or other imaging studies. If the fracture involves the anterior (front) part of a vertebral body more than the rest of the vertebra, the spine will tend to curve forward and result in the popularly known dowager’s hump.
Compression fractures are graded in regard to the percent of the vertebra that is compressed, compared to the normal height of the vertebra. Normal height is judged from adjacent vertebrae. Pain, loss of motion, and muscle spasm are most likely to be present at the time of fracture and in the healing period. Marked or multiple compression fractures are more likely to produce chronic pain.
Plain X-rays are much less sensitive than bone densitometry in determining the severity of osteoporosis. A normal appearance of bone on plain X-rays only rules out the most advanced osteoporosis. Plain X-rays are fine for determining the percentage of vertebral body collapse in compression fractures.
Trauma
Fractures of the bony spine are most commonly related to automobile or motorcycle accidents. There may be associated spinal cord injury. Traumatically fractured vertebrae are treated with a combination of surgical fusion and sometimes stabilization with metal rods.
Tumor
The most serious tumors of the spine arise from cancer that has spread to the spine from breast, colon, prostate, or other origin. Tumors can not only cause chronic pain, but result in spinal fractures as they destroy bone. The spread of cancer of any kind to the spine is a serious development that must also be considered under the listings dealing with cancer.
Arachnoiditis
Arachnoiditis is inflammation of some part of the arachnoid membrane that covers the spinal cord. It can produce severe chronic pain. Arachnoiditis may occur as a result of infection, but most commonly is seen after surgical procedures and use of contrast material to enhance visualization of structures with X-rays during myelography. Some people are more sensitive than others to contrast material. An MRI scan has about a 90% chance of showing this abnormality if it is present. A negative MRI scan for arachnoiditis is a strong argument that it is not present.
Lumbar Strain
Lumbar strain refers to stress on the ligaments, muscles, and other soft tissues near the spine with resultant pain. There may or may not be underlying arthritis or DDD. Acute strain, associated with a particular lifting event, will almost always resolve in several months. If the pain is marked, there is associated muscle spasm and difficulty bending the back. When back pain continues for a prolonged period, orthopedists and other doctors tend to apply the diagnosis of “chronic lumbar strain,” if there is no other underlying identifiable abnormality that can be seen on imaging studies.
Spondylolisthesis
Spondylolisthesis is a slippage of vertebral bodies out of their normal position, usually a forward slippage of the 5th lumbar vertebra over the 1st sacral vertebra (L5-S1). More rarely, a type of spondylolisthesis called retrolisthesis involving the backward displacement of a vertebral body occurs. Most spondylolisthesis is seen in the lumbar spine (L1-L5/S1). This disorder can been seen on plain X-rays. It is significantly more likely to be seen on X-rays taken in the standing position than in those taken in lying position—with weight on the spine, slippage is more likely.
However, severe or even significant neurological abnormalities (sensory changes, reflex changes, muscle weakness or atrophy) are not to be expected in spondylolisthesis.
Studies have shown that most individuals with spondylolisthesis, lead active lives with little, if any, adjustment for having this type of spinal abnormality. Spondylolisthesis is most likely to become limiting as a contributing factor for spinal stenosis in combination with other spinal disorders, such as severe osteoarthritis and severely bulging intervertebral discs.
Spinal Stenosis
Spinal stenosis is a narrowing of the space inside the bony spine (see Figure 7 below), which sometimes results in pressure on the spinal cord and peripheral nerve roots from the spinal cord. The Social Security Administration most commonly sees such cases in claimants who have severe osteoarthritis of the lower spine. Spinal stenosis can be worsened by bulging or herniated disks (HNPs) (see Figure 8 below) and spondylolisthesis.
Spinal stenosis most commonly involves the lower back, specifically the area somewhere between the 3rd lumbar vertebra and the beginning of the sacrum (L3-4, L4-5, and L5-S1 levels). Less frequently, the neck (cervical spine) may be involved with spinal stenosis; its presence in the upper back (thoracic spine) is rare.
Spinal stenosis is one of many possible causes of damage to the spinal cord (myelopathy). Myelopathy may be irreversible. Surgical decompression of the spinal cord may be necessary for severe cases, but even after surgery symptoms may not improve.
Pain and neurological abnormalities can be debilitating if treatment is not effective. Standing, walking, lifting, and carrying should be limited to weight that does not produce symptoms. A person with lumbar stenosis may have no symptoms during a physical examination, but may have severe symptoms with exertion.
Pain, weakness, numbness or other symptoms related to spinal stenosis usually appear gradually over a period of months or years. Symptoms are rapidly worsened by walking, lifting, jarring, carrying or other activities that strain the spinal structures. Sensory abnormalities, such as numbness, will occur before the onset of weakness. Symptoms are lessened or relieved by bending forward (including crouching) or lying. These symptoms are referred to as pseudoclaudication by the Social Security Administration, but are often also called neurogenic claudication.
In addition to osteoarthritis, causes of spinal stenosis include congenital spinal deformities (scoliosis, kyphosis, or congenital skeletal dysplasias like achondroplastic dwarfism); acquired deformities such as post-traumatic spinal fractures; inflammatory spinal diseases like ankylosing spondylitis; or stenosis may be of unknown cause. Tumors or infection present possible reversible causes of lumbar stenosis.
Spinal stenosis can be seen on imaging studies such as myelography, CT, and MRI scans. But myelography and CT scans can miss some types of stenosis.
Scoliosis
Scoliosis is a sideways curvature to the spine (see Figure 9 below), associated with pain but not neurological impairment. Scoliosis can be of any degree of severity. Often the scoliosis is associated with one leg being shorter than the other. In these instances, the pelvis is not level causing the abnormal sideways spinal curvature. Scoliosis should be suspected with leg length discrepancies of 2.2 cm or greater.
The abnormal spinal curve of scoliosis is measured on plain X-rays. The measurement is called a Cobb angle. Scoliosis may be considered present with abnormal curves greater than 10 degrees. Mild cases have angles less than 30 degrees.
Angles of 20 degrees or less are usually produce no symptoms. Bracing is prescribed for angles over 20 degrees. Curves over 40 degrees may produce neurological abnormalities such as sensory loss and weakness. Small curves of less than 30 degrees in childhood are not likely to get worse during adulthood, while more severe curves may continue to progress. Surgery with permanent rod implantation and fusion is indicated with curves greater than 45 degrees.
Claimants with curves 60 degrees or more require spirometry for restrictive lung disease (decreased vital capacity). See Can I Get Social Security Disability Benefits for Lung Disease? Heart failure may occur from scoliosis when abnormal curves are markedly severe at 100 degrees or more. Such cases are very rarely seen in Social Security disability adjudication.
During physical examination, a doctor may use a device known as a scoliometer (scoliosometer) to measure the degree of curvature. The scoliometer measurement should not be confused with the spinal curvature, although both are expressed in degrees. A scoliometer reading of 7 degrees corresponds to a 20-degree curve measured by Cobb angle on X-ray. Scoliometers are inexpensive and useful for screening, but direct curve measurements on plain X-ray views are needed for accurate determinations.
Kyphosis
Kyphosis is an abnormal degree of curvature of the thoracic spine (upper back) in the forward direction (flexion). Kyphosis may be congenital or may occur in post-menopausal osteoporosis with collapse of the anterior (front) part of vertebral bodies in the upper back.
In kyphosis, forward curvature of the spine up to 20 degrees is considered normal, and mild up to 40 degrees. Bracing is prescribed for angles over 40 degrees and balance can be impaired by kyphotic curves greater than 40 degrees. Curves of 50 degrees or greater can produce a significant restrictive breathing deficit and should have vital capacity tested with spirometry. See Can I Get Social Security Disability Benefits for Lung Disease? As with scoliosis, extremely abnormal curves of 100 – 110 degrees or more can compromise cardiac function.
Osteomyelitis
Osteomyelitis most often occurs as a result of trauma producing open wounds that allows the entry of bacteria into the body, as a result of surgical procedures, or as a result of bacteria circulating in the bloodstream—a condition known as bacteremia. Osteomyelitis of joints can affect their function by means of bone destruction and joint deformity. See Can I Get Social Security Disability Benefits for Arthritis or Joint Damage?
In weight-bearing bones, fractures through the area of infection can occur during the stage of acute infection, or later due to brittle bone. The orthopedic surgical management of osteomyelitis can be complex. Surgery may be needed to remove infected bone.
With modern antibiotics, acute osteomyelitis can be treated more effectively, so that chronic osteomyelitis is not as common as it was in the past. When chronic osteomyelitis does occur, it can present a difficult problem because the chronically infected bone may die and that restricts delivery of antibiotics through the bloodstream. Also, secondary infection may occur in tissues near the bone that involves different organisms than those that infect the bone itself.
An area of infected bone is called a sequestrum. In the treatment of chronic osteomyelitis, surgery to remove the sequestrum (sequestrectomy and curettage) along with infected soft tissues near the infection is a common requirement. Infected soft tissue removal may require reconstruction of soft tissues, such as muscle and skin grafts. The hole in the bone left by removal of the sequestrum may be packed with antibiotic beads. Antibiotic bead implantation may be temporary (10 days) to permanent, depending on the judgment of the surgeon. Whatever surgical antibiotic treatment is given, the patient will require prolonged systemic antibiotic therapy lasting well through surgical recovery, in order to prevent recurrent infection.
Infected bone fractures can be particularly difficult to heal. Such a situation might arise from an open wound and fractures occurring during an automobile accident or other trauma.
Winning Social Security Disability Benefits for Back Problems by Meeting a Listing
To determine whether you are disabled at Step 3 of the Sequential Evaluation Process, the Social Security Administration will consider whether your back problems are severe enough to meet or equal the listing for spine disorders. The Social Security Administration has developed rules called Listing of Impairments for most common impairments. The listing for a particular impairment describes a degree of severity that Social Security Administration presumes would prevent a person from performing substantial work. If your back pain or mobility is severe enough to meet or equal the listing, you will be considered disabled.
Most claimants with back problems do not qualify for Social Security disability benefits under the listing, and require a residual functional capacity assessment. See Residual Functional Capacity Assessment for Back Pain.
The listing for spine disorders is 1.04. It has 3 parts: A, B, and C. You will meet the listing and be eligible for Social Security disability benefits if you meet any of the three parts.
Meeting Social Security Administration Listing 1.04A for Disorders of the Spine
You will meet listing 1.04A if you have:
- A disorder of the spine (e.g., herniated nucleus pulposus, spinal arachnoiditis, spinal stenosis, osteoarthritis, degenerative disc disease, facet arthritis, vertebral fracture);
- Resulting in compromise of a nerve root (including the cauda equina) or the spinal cord (see Figure 10 below);
- With evidence of nerve root compression;
- Characterized by–
- neuro-anatomic distribution of pain,
- limitation of motion of the spine
- motor loss (atrophy with associated muscle weakness or muscle weakness) accompanied by sensory or reflex loss, and
- if there is involvement of the lower back, positive straight-leg raising test (sitting and supine).
Bone spurs, herniated disks, cancerous or benign tumors, arachnoiditis, or other abnormalities may put pressure on a spinal nerve root. Most of these problems occur in the lumbar spine, especially the intervertebral disk between the 5th lumbar vertebra and the lower vertebra. CT and MRI scans can provide non-invasive and accurate diagnosis of herniated disks and other disorders impinging a nerve root, but image results do not necessarily imply a particular level of symptoms or severity.
“Motor loss” refers to muscle weakness as objectively determined by measurement of muscle size to determine if there is muscle wasting (atrophy). While atrophy is more convincing evidence of severe nerve root compression than weakness alone, part A clearly specifies that muscle weakness alone is sufficient. Thus, for example, a claimant’s ability to walk on the left toes and not the right toes would indicate significant right calf weakness.
Changes in deep tendon reflex (DTR) will occur if there is pressure on a nerve root. Most reflex changes are related to arthritic spurs or a herniated disk (HNP) pressuring a nerve root as it leaves the spinal cord. In these instances, reflexes related to the part of the body that the nerve root serves (the “radicular distribution”) will be decreased (hypoactive). Similarly, sensation in that body area (sensory dermatome) may be decreased because of injury to nerve fibers.
It is almost impossible to satisfy this part of the listing for several reasons. Often, a person has an acutely painful herniated disk (HNP) but no significant neurological changes; especially lacking are the classical findings of sensory, motor, and reflex changes that are required. If a person has these abnormalities, he or she is extremely likely to have surgery to relieve significant nerve root compression. Once surgery is done to decompress a nerve root, scarring around the nerve root may be a source of some degree of chronic pain. However, the persistence of reflex and sensory abnormalities after surgery is not proof of ongoing nerve root compression.
Meeting Social Security Administration Listing 1.04B for Disorders of the Spine
You will meet listing 1.04B if you have:
- A disorder of the spine (e.g., herniated nucleus pulposus, spinal arachnoiditis, spinal stenosis, osteoarthritis, degenerative disc disease, facet arthritis, vertebral fracture),
- With spinal arachnoiditis,
- Confirmed by an operative note or pathology report of tissue biopsy, or by appropriate medically acceptable imaging,
- Manifested by severe burning or painful dysesthesia, resulting in the need for changes in position or posture more than once every 2 hours.
The preferable “acceptable imaging” for part B is MRI. Plain X-rays and CT scan X-rays of the spine cannot image the soft tissues well enough to provide any useful information regarding arachnoiditis.
It helps your claim greatly if your treating physician provides longitudinal medical records supporting the allegation of painful dysesthesia (impairment of the sense of touch) and your need to change position or posture more than once every 2 hours. The Social Security Administration should try to obtain the needed information regarding your time-tolerance for body position and posture from your treating doctor, if the medical records are not clear. A detailed analysis of your activities of daily living (ADLs) can also be helpful. It is important that you provide specific examples of the pain and your need to change positions. The Social Security Administration should ask you clear questions that elicit these examples.
Changes in body position or posture need to be significant, like the need to stand up or sit down—not merely moving around in a chair a little to get more comfortable.
Meeting Social Security Administration Listing 1.04C for Disorders of the Spine
You will meet listing 1.04C if you have:
- A disorder of the spine (e.g., herniated nucleus pulposus, spinal arachnoiditis, spinal stenosis, osteoarthritis, degenerative disc disease, facet arthritis, vertebral fracture),
- With lumbar spinal stenosis resulting in pseudoclaudication (pain and weakness usually in the low back and buttocks),
- Established by findings on appropriate medically acceptable imaging,
- Manifested by chronic nonradicular pain and weakness,
- Resulting in inability to ambulate effectively.
Inability to ambulate effectively means an extreme limitation of the ability to walk. Ineffective ambulation is defined generally as having insufficient lower extremity functioning to permit independent ambulation without the use of a hand-held assistive device(s) that limits the functioning of both upper extremities. To ambulate effectively, you must be capable of sustaining a reasonable walking pace over a sufficient distance to be able to carry out activities of daily living. You must have the ability to travel without companion assistance to and from a place of employment or school. Therefore, examples of ineffective ambulation include, but are not limited to:
- The inability to walk without the use of a walker, two crutches or two canes,
- The inability to walk a block at a reasonable pace on rough or uneven surfaces,
- The inability to use standard public transportation,
- The inability to carry out routine ambulatory activities, such as shopping and banking, and
- The inability to climb a few steps at a reasonable pace with the use of a single hand rail.
The ability to walk independently about your home without the use of assistive devices does not, in and of itself, constitute effective ambulation.
Spinal stenosis is not rare, but can be missed by the Social Security Administration if your medical records consist only of a physical examination and plain X-rays. That’s why the examining doctor should take a careful history to rule out the symptoms of pseudoclaudication that might be caused by spinal stenosis. If you have severe lower lumbar arthritis and symptoms of pseudoclaudication, then the Social Security Administration should send you for a lumbar CT scan or MRI, if one has not been done. The Social Security Administration wants confirmation of lumbar stenosis on imaging, but provides no guidance regarding what is acceptable as diagnostic of abnormality. Measurements on imaging procedures that are diagnostic of lumbar stenosis have not been established in the medical literature. Therefore, the Social Security Administration must be willing to accept this imaging diagnosis as a matter of judgment by the interpreting radiologist, orthopedic surgeon, or neurosurgeon.
“Nonradicular” pain means the pain does not have to follow the pattern of a particular nerve root; it can occur more diffusely in the buttocks, back, or thighs.
As in other types of back impairments, careful development of your daily activities and the opinion of your treating physician are critical in deciding whether you satisfy the listing in regard to effective ambulation, once the diagnosis is established.
If your spinal cord is damaged enough to cause significant neurological abnormalities (a possibility with spinal stenosis), the affected deep tendon reflexes (DTRs) are expected to be abnormally brisk (hyperactive). For example, eliciting the knee-jerk reflex will cause your leg to move with a quicker than normal reaction. Contrast this to damage to a spinal cord nerve root as from a herniated disk, in which the affected DTR will be slower than expected. However, unlike part A of the listing that deals with nerve root compression, part C does not require reflex abnormalities to be present. In spinal stenosis, reflex changes are specific enough to be diagnostic.
Residual Functional Capacity Assessment for Back Pain
What Is RFC?
If your back injury is not severe enough to meet or equal a listing at Step 3 of the Sequential Evaluation Process, the Social Security Administration will need to determine your residual functional capacity (RFC) to decide whether you are disabled at Step 4 and Step 5 of the Sequential Evaluation Process. RFC is a claimant’s ability to perform work-related activities. In other words, it is what you can still do despite your limitations. An RFC for physical impairments is expressed in terms of whether the Social Security Administration believes you can do heavy, medium, light, or sedentary work in spite of your impairments. The lower your RFC, the less the Social Security Administration believes you can do.
Neck Abnormalities
Individuals with spine abnormalities involving the cervical spine (neck) are not as limited as those involving the lumbar spine (lower back). The ability to perform overhead work is often limited and can be an important consideration. However, the overhead work restriction is not limited to cervical fusions. An fusion of the cervical spine caused by arthritis would have the same effect, as would any condition of the cervical spine that results in painful movement and stiffness, like the inflammatory spondyloarthropathies (e.g., ankylosing spondylitis), or simply advanced osteoarthritis.
The Social Security Administration is liable to overlook rotational movement ability in the neck as an important work-related limitation. Even less regard is given to rotational ability in the lower spine. While these functions are not as important as bending and the ability to look upward, they could be a critical in some claims—especially the ability to look right and left without having to turn the whole body.
Spondylolisthesis
Grade I spondylolisthesis is rarely symptomatic and often found incidentally on X-ray. Grade I patients generally do not receive any restrictions from orthopedic surgeons. As a generalization, symptomatic grade II spondylolisthesis can result in restriction to medium work; grade III restriction to light work; and grade IV can sometimes be limited to sedentary work. However, this degree of functional severity is unusual and refers only to those rare cases with significant symptoms.
Spondylolisthesis is an anatomical abnormality that does not, by its mere appearance on imaging studies, imply symptoms or functional limitation. For example, some studies over a period of years showed no symptoms in over a third of patients followed with grades III and IV spondylolisthesis, and only mild symptoms in over half of the cases with grade IV slippage.
Of course, all cases must be evaluated in light of the individual claimant’s symptoms. Persistent, significant back pain related to spondylolisthesis and not responding to conservative treatment is likely to be treated with lumbar fusion.
Laminectomies
In uncomplicated cases of an HNP (herniated disc) and treatment with a surgical discectomy (see Figure 11 below) and laminectomy, the Social Security Administration will generally tend toward giving a medium RFC with occasional bending. If there are additional problems, such as associated arthritis elsewhere in the spine, surgery at multiple levels, or persistent pain, then the RFC should be lower. The important point is that the Social Security Administration should give no higher than a medium RFC (lifting up to 50 lbs) if modest pain persists. The most appropriate RFC for an individual claimant may be lower. A completely asymptomatic claimant after a simple laminectomy might receive no restriction in regard to back impairment.
Generally speaking, the Social Security Administration considers a 3 to 4 month recovery period sufficient for cases involving post-operative laminectomy or spinal fusion. This is true only in the absence of complications.
Cervical or Lumbar Fusion
In cases of trauma, or the need of stabilization to alleviate chronic pain, the spine may be surgically fused (see Figure 12 below). In these cases, the Social Security Administration is likely to give no higher than a medium RFC with occasional bending even in cases of optimum post-surgical recovery. Those with any significant chronic pain generally receive no higher than a light RFC with occasional bending.
Figure 12: Vertebral fusion involving placement of a bone graft into a hollowed out disc space.
Fusions of the cervical spine are less limiting in regard to lifting and carrying, since they are not in the weight-bearing part of the spine. However, lifting heavy weights can put traction on the cervical spine through the back and neck muscles, resulting in symptoms. In other words, the lack of pain or other symptoms during resting physical examination does not imply the absence of limitation at heavier work-loads.
Some claimants who have had a fractured and unstable cervical spine during an accident, may warrant no higher than a sedentary RFC, if there is risk of death or spinal cord injury from heavier work. Also, there may be a residual neurological deficit from spinal cord injury at the time of injury, in the case of the accident.
In other instances, a decompressive cervical laminectomy and fusion is necessary to relieve spinal stenosis pressure on the cervical spinal cord. These cases are likely to require more limitation than those with a simple, uncomplicated cervical fusion. If the claimant has had pain lifting during his or her activities of daily living or attempt to return to a prior job, it is important that this information be documented in his or her disability file. Furthermore, cervical fusions can make it impossible for a person to perform overhead work, which can be a critical limitation in some cases.
Location of Arthritis
Generally speaking, arthritis occurring in the thoracic spine is not as symptomatic or functionally limiting as arthritis in the lumbar or cervical spine. Similarly, cervical spine arthritis is not as limiting as that in the lumbar spine of the same severity. Of course, individual cases may differ.
Osteoporosis
Claimants who do not meet the listing still may have limitations imposed by osteoporosis. Many post-menopausal women have osteoporosis of the spine but do not have the generalized osteoporosis required by the part B of the listing.
In the absence of generalized osteoporosis and the presence of a 50% compression fracture and symptoms of back pain, the Social Security Administration will generally agree that a RFC is no higher than medium work and could be lower—especially if there are multiple fractures.
Some spinal osteoporosis can be so severe that, when viewed with even plain X-rays, the vertebral bodies have an obviously thinned out ghost-like appearance. These claimants may be restricted to as low as sedentary work, based on the obvious conclusion that to lift more than minor weight would likely cause spinal fractures. Sometimes, it is important for Social Security Administration doctors to obtain X-rays from the source and look at the images themselves. If there is any question about the severity of the osteoporosis, the Social Security Administration should obtain bone densitometry for a more accurate measurement.
Spinal Stenosis
In cases of spinal stenosis that are not severe enough to satisfy the listing, the Social Security Administration should nevertheless take care that the RFC given does not result in symptoms. The important questions are:
- How much weight can you lift and carry, both frequently and occasionally, without symptoms?
- How long can you walk or stand?
If standing or walking is limited to less than 6 to 8 hours daily, then you are automatically restricted to sedentary work. It is important to ascertain the difference between standing and walking while carrying nothing and while carrying something. For example, a claimant with symptomatic lumbar stenosis may be able to stand or walk 6 to 8 hours, but not necessarily while carrying 20 lbs. In that instance, the RFC would be restricted to sedentary work. Careful case development of the claimant’s symptoms is necessary to determine RFCs in these cases.
It is difficult to assess how far a person can walk or how much a person can lift just by looking at imaging studies showing the anatomical severity of spinal stenosis. Greater weight should be given to alleged symptoms and limitations in activities of daily living than trying to guess RFC from imaging results. The only exceptions might be in highly atypical cases where, for example, a claimant with extremely mild spinal stenosis—perhaps borderline abnormal—alleges marked limitations.
Artificial Intervertebral Disks
Artificial spinal disk implants are not yet common enough to know how well they will permit repeated flexion of the spine on a day-to-day basis. It is also unknown what weights patients will reasonably be able to lift frequently or occasionally, or lift and carry. Larger studies with many more patients will be required to answer those questions. At the present time, it would seem reasonable to restrict lumbar, single artificial disk patients to no more than light work—provided there is no functional information to the contrary—with occasional bending. It is less clear what RFC is reasonable in a person with a single, cervical artificial disk since that part of the spine is not as weight bearing. These cases should never be assessed as “not severe” (slight). Furthermore, multiple artificial disks—regardless of their location—would warrant no higher than a light RFC. Of course, significant symptoms could decrease these capacities.
Vertebroplasty
Vertebroplasty involves stabilizing fractured vertebrae with glue (polymethylmethacrylate, PMMA), also referred to as “bone cement.” It was first used in 1984 to treat compression fractures caused by cancer, and since 1994 has been used to treat osteoporotic compression fractures. Vetebroplasty is a common procedure. The glue is injected under local anesthesia, with resulting improvement in spinal mobility and back pain in about 96% of patients. The pain relief is often very substantial with a corresponding increase in function and the quality of life. It would seem reasonable that osteoporosis requiring vertebroplasty for compression fractures would limit the RFC to no higher than light work to avoid additional fractures.
Chronic Back Pain after Multiple Surgeries
Some claimants have severe spinal arthritis, multiple surgeries, and persistent chronic pain both sitting and standing. Multiple back surgeries are particularly notorious for causing chronic back pain problems and these claimants may show scarring around nerve roots on CT or MRI. Such scarring may be the only rational basis for alleged persistent pain. Cases of severe persistent back pain are unusual but not rare, and require careful medical judgment to determine if the claimant’s residual functional capacity precludes even sedentary work. The claimant may be restricted to sedentary work, and have to frequently alternate sitting and standing. In that event, the claim is almost always allowed since it is difficult to find jobs that a person with that kind of limitation can do. Critical in this determination is not only the objective medical evidence, but consideration of the treating doctor’s opinion and the claimant’s activities of daily living (ADLs). The credibility of the claimant’s pain-related allegations increases substantially when there is a well-documented interaction with the treating doctor in which the claimant describes and attempts to get relief for pain. Particularly important is the treating doctor’s opinion about how long he or she thinks the claimant can sit or stand in any one period of time as well as on a total daily basis.
If a claimant is otherwise limited to sedentary work and also unable to sit at least two hours in one period without standing, it would be difficult for the Social Security Administration to cite a job the claimant can perform. It is important for the treating doctor to rationalize to the Social Security Administration why severe functional limitations are present, for example, to refer to the medical evidence showing objective abnormalities and provide the findings of a careful physical examination.
Medical Opinion Forms
Medical opinion forms can be great time savers for both your advocate and your doctor, but they must be used with care. Forms may not be appropriate at all in complex cases; and they need to be supplemented in many cases so that all issues are addressed. The best forms are clear and complete but not too long.
When the time is right, here is a form for your disability advocate to use:
Spinal_Disorder_Data_Sheet
Kim Engler / Disability Advocate

Disability Advocates Group has been championing the cause of the disabled for over 20 years. We view each claim as a unique challenge and entitled to individualized strategy to help ensure a successful outcome. Remember, we don’t get paid unless you get paid!